【新冠抗疫】一名ICU研究护士的工作日记
Lauran O’Neill is a Senior Research Nurse in the critical care research team. She’s worked at Great Ormond Street Hospital for around 15 years in total, but has never been more busy and proud of her colleagues than in the last two months. This is her experience of COVID-19 so far.
Late March 2020: Okay, what just happened?
Things feel a little stalled right now. There’s a strange, expectant atmosphere at GOSH. In our team there’s massive uncertainty about what we’re going to be doing. Most of our research studies are suddenly on pause, except ones that are part of essential treatment.
Because most of us have backgrounds in intensive care nursing, it looks like we might be deployed to clinical areas to look after patients. We’re looking at what training we need to pick up those roles again. I’m actually really looking forward to going back. I want to be as useful as I can, and I love being at the bedside, making connections with patients and their families.
I’ll miss research though. I’ve really fallen in love with it over the past few years, since I moved over from a clinical role in ICU. I love seeing how research leads to changes in the way we do things at the bedside.
Coming into work every day, I am worrying about exposing my family to the virus. I’ve got two young children at home, plus my mum and my husband, who’s also an essential worker. But the way I’m seeing it is I'm probably in as good a position as anyone to do the job, and I'm super passionate about it. So at the minute, weighing up the stress and the risk, versus not doing the job - it feels worth it. And my family are super supportive and proud. That really helps.
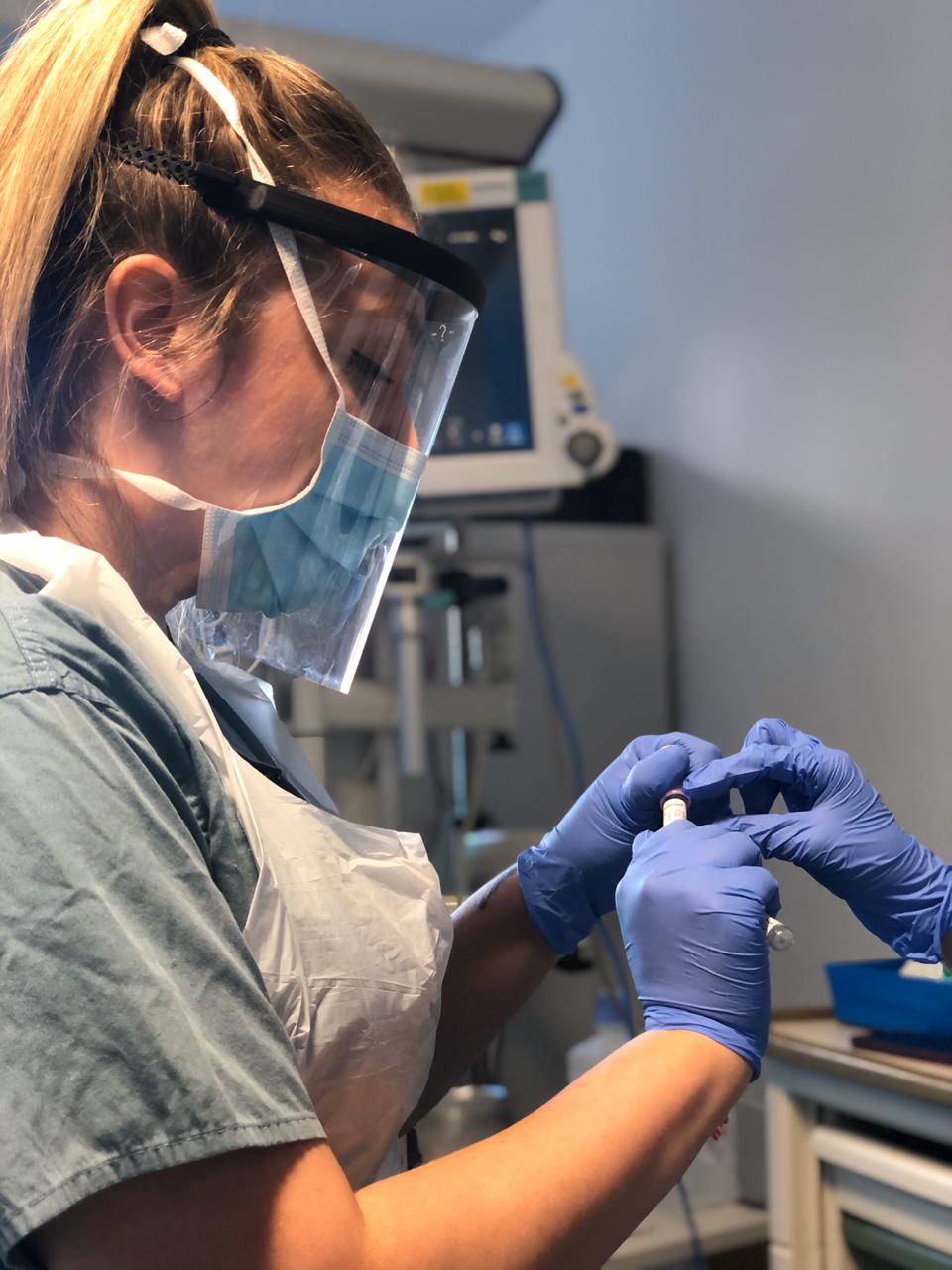
Early April 2020: COVID research explodes
Our workload has exploded in the space of two weeks. The intensive care units ended up being well staffed, so we weren't needed in clinical roles. We started migrating back to our research roles and thank goodness we did, because suddenly the COVID research studies are coming in thick and fast.
There are loads being set up across GOSH, some part of national studies and others more bespoke to GOSH looking at how COVID-19 affects children with underlying conditions. The pace people are coming up with new ideas is incredible.
Usually, when we set up a research study, it takes at least a couple of months for everyone to understand how it will run and plan for every eventuality. Now, we’re getting information on a Monday and by Thursday we’re opening the study and recruiting patients.
It’s intense, but the team have been amazing. They're used to working at a fast pace anyway, but they’ve had new information brought to them so quickly and they’re getting things in motion in record time. In the future, I think this will be something to look back on and be incredibly proud of.
We’re used to spending all our time on ICU, so it’s been an adjustment working across the whole hospital. But we are meeting lovely new ward staff and seeing children in environments where they are recovering, which is fantastic.
Mid April: A typical day
We’re beginning to settle into a strange new normal. The mornings are particularly hectic. We come in at 7am and use our electronic patient record system – EPIC – to find any new patients that are eligible for the COVID-19 studies we’re running. It’s an amazing system! You can filter through all the patients in the whole hospital in the blink of an eye.
Then we speak to each patient’s clinical consultant and their bedside nurse, to check the family are aware of the COVID-19 diagnosis and that it isn’t a bad day for us to speak to them.
Quite quickly after that, we speak to the family about whether they’d like to join the study. The two COVID-19 studies we’re running now require additional samples to be taken, so we don’t take it lightly asking children and their parents to take this on. We have to be super sensitive to the journey that they're on, given how scary things seem right now and the fact that their child is in hospital, not only with COVID-19 but often other significant health issues.
We give them information about the study, but leave them for a couple of hours so they can think about it. We make sure we give the information in a way that they can digest and understand. Later we come back to see what they’ve decided. It’s very much a conversation, making sure the family understands the research and its risks. For those who choose to join the study, we go back pretty quickly to get the first samples. We’ll need to take the same samples every day, to keep track of how their body is reacting to the infection and any treatment.
The samples need to be in the GOSH labs by 3pm, so it’s an intense turnaround with loads of different teams involved.
When we’ve handed in our samples we stop, get a cup of tea, and catch up with paperwork. It’s nice to come together with the rest of the team after we’ve all been running around the hospital non stop.
Late April 2020: One month in
Can I just say, the free coffee cart for staff has been a genuine lifesaver. It’s just around the corner from the main hospital canteen, but it’s a space just for staff and as soon as I stand in that queue, I can feel myself relax. They're really nice guys behind the counter, so friendly. And to not have to pay is an added bonus. Also, the quality of the coffee is incredible! Massive thank you everyone who donated to GOSH Charity - you helped make it happen!
We’re finding that the vast majority of families are saying yes to joining our COVID-19 studies. Every day this floors me. They are so willing to help other parents and children in the future by participating in a study, that they’re prepared to undergo additional sampling and therefore probably more discomfort for the patient, even though it won’t offer immediate benefits for their own child.
When we speak to families, it’s often day one of their child’s COVID diagnosis. They've already had so much information thrown at them and they must be so worried. Yet still, at their most vulnerable point, they have the capacity to think of other people. For our team, it's nice to be part of that.
Early May 2020: Smiling with your eyes
On some wards, we need to wear full PPE as we consent patients and take samples – that means mask, visor, gloves and full gown. The heat is unreal when you’ve got all the kit on. I was trying to talk to a parent today and thinking 'try not to pass out'. I don't know how some of the clinical staff are doing 12 hours in this kit.
It has changed a lot for us, day to day. Little things you usually take for granted, like eye contact, body language, touching a mum’s arm or them seeing you smile. It’s not as easy to rely on those now to connect with families, comfort them or put them at ease. A mum might say she's okay, but we’re used to picking up on small cues that might suggest she’s struggling. It’s much harder to do that now. But I’ve seen incredible compassion from the nurses across GOSH. They’re visibly putting in that extra effort to make sure families get proper human support and connection.
I find myself doing these insane smiles when I’m in PPE. I’d look absolutely crazy without the mask on! But because they can only see my eyes, I want to be sure they can see that I’m smiling.
It's five o'clock on Friday right now and I haven't seen anyone else from my team today. We’ve been running all over the hospital consenting patients for studies. But I’m smiling because I’m looking at some beautiful, knitted drawstring bags that have just been delivered to the nurses on PICU. Some amazing people have sat at home and hand sewn them. It’s just incredible how practical some of the gifts we’ve had are. A nurse can pop their uniform in this bag, go home and put the whole thing straight in the wash. In the midst of everything that’s happening, the generosity and support of absolute strangers has, for me, been the most astounding thing.


