Mr Greg James
Overview
Greg James is a Paediatric Neurosurgeon with clinical and research specialisms in craniofacial surgery, cerebrovascular surgery, complex cerebrospinal fluid (CSF) disorders, stereotactic radiosurgery and head injury.
His surgical philosophy is built on three tenets:
-
Excellent surgical technique - augmented by the most advanced technology for safety and efficacy
-
Teamwork - with high volume, subspecialized multidisciplinary groups such as the Great Ormond Street Hospital Craniofacial Unit and Neurovascular Team
-
Open, honest and full communication with children and families at all stages of their clinical journeys. He encourages families to contact him directly with questions and values open discussion about the pros and cons of surgical decisions.
In addition, he strongly believes surgical and academic excellence go hand-in-hand and regularly presents and publishes research internationally, as well as holding multiple local and national neurosurgical training roles. He is honorary Senior Lecturer at University College London, as well as honorary Consultant Neurosurgeon at the National Hospital for Neurology and Neurosurgery.
Credentials
- Craniosynostosis (simple and complex)
- Craniofacial tumours/trauma
- Minimally invasive craniofacial surgery including endoscopic + helmets
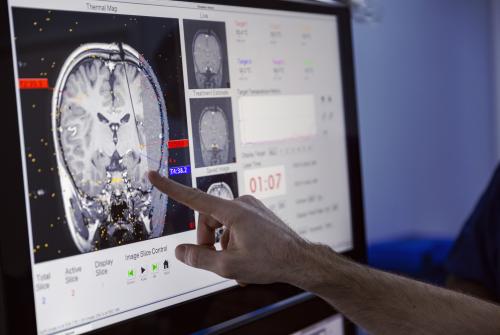
- Gamma Knife stereotactic radiosurgery
- Cerebrovascular disease
- Arteriovenous malformation
- Cerebral aneurysm
- Cavernoma
- Occlusive arterial disease – stroke, moyamoya
- Hydrocephalus (including difficult shunts and ETV/CPC shunt avoidance surgery)
- Neuro-endoscopy
- Neonatal neurosurgery
- Intracranial pressure
- Antenatal counselling
- Craniofacial Surgery - including minimally invasive surgery including endoscopic suturectomy/helmeting and spring-assisted cranioplasty
- Cerebrovascular Surgery - including combined endovascular/microsurgical AVM resection, cavernoma, revascularisation
- Complex CSF disorders - including ETV-CPC, difficult shunt problems, arachnoid cysts, neuro-endoscopy
- Stereotactic radiosurgery - Gamma Knife for AVMs and tumours in children. He is Lead at the Children’s Gamma Knife Centre at GOSH/UCLH
- Head injury - particularly complex craniofacial reconstruction
Qualifications:
- BSc in physiology, First Class Honours (London 1999)
- MBBS with distinction (London 2004)
- PhD in neuroscience (London 2014)
- Membership of Royal College of Surgeons of England (2005)
- Fellowship of Royal College of Surgeons of England (Neurosurgery, 2013)
- Specialist Registration in Neurosurgery (2014)
- European Society of Paediatric Neurosurgery Course (three year cycle completed 2015)
- Leksell Gamma Knife Course (Marseilles 2017)
Memberships:
- Society of British Neurological Surgeons
- European Society of Paediatric Neurosurgery
- British Paediatric Neurosurgery Group
- British Neurovascular Group
- British Radiosurgical Society
His current projects include:
• The management of intraventricular haemorrhage in preterm infants
• Techniques for fronto-orbital remodelling in single suture synostosis
• The relationship between disordered sleep and intracranial pressure in children with craniosynostosis
• Surgical techniques for reducing shunt infection and dysfunction in children
• Improving pathways of care and patient safety in craniofacial surgery
• Management of arteriovenous malformations in children
News & Publications
Ozoani, G., Sharma, J.D., Wahab, S., Aquilina, K., James, G. 2017. Antenatally diagnosed pre-pontine arachnoid cysts with significant post-natal supratentorial progression: report of two cases. Child's Nervous System.16 pp. 1–3.
James, G., Thompson, D.N.P. 2017. Atlanto-axial rotatory fixation: a serious potential complication of paediatric ENT surgery that requires prompt diagnosis and treatment. The Journal of Laryngology and Otology. Cambridge University Press. ep 1(30) pp. 1–6.
Borghi, A., Schievano, S., Rodriguez-Florez, N., McNicholas, R., Rodgers, W., Ponniah, A., et al. 2017. Assessment of spring cranioplasty biomechanics in sagittal craniosynostosis patients. Journal of Neurosurgery: Pediatrics. 25 pp. 1–10.
Bowes, A.L., King-Robson, J., Dawes, W.J., James, G., Aquilina, K. 2017. Neuroendoscopic surgery in children: does age at intervention influence safety and efficacy? A single-center experience. Journal of Neurosurgery: Pediatrics. 28 pp. 1–5.
Rodriguez-Florez, N., Ibrahim, A., Hutchinson, J.C., Borghi, A., James, G., Arthurs, O.J., et al., 2017. Cranial bone structure in children with sagittal craniosynostosis: Relationship with surgical outcomes. British Journal of Plastic Surgery. Elsevier Ltd. 19 pp. 1–9.
Copley, P., Kirkman, M.A., Thompson, D., James, G., Aquilina, K. 2017. Endoscopic surgery for intraventricular arachnoid cysts in children: clinical presentation, radiological features, management, and outcomes over a 12-year period. Child's Nervous System. 14 pp. 1–10.
Rodgers, W., Glass, G.E., Schievano, S., Borghi, A., Rodriguez-Florez, N., Tahim, A., et al., 2017. Spring-Assisted Cranioplasty for the Correction of Nonsyndromic Scaphocephaly: A Quantitative Analysis of 100 Consecutive Cases. Plastic and Reconstructive Surgery. 140(1) pp.125–34.
Rodriguez-Florez, N., Bruse, J.L., Borghi, A., Vercruysse, H., Ong, J., James, G., et al., 2017. Statistical shape modelling to aid surgical planning: associations between surgical parameters and head shapes following spring-assisted cranioplasty. Int J Comput Assist Radiol Surg. Springer International Publishing. 26 pp. 1–11.
Ogborne, R., Spoor, J., James, G. 2017. Haemorrhage into a cavernoma after traumatic head injury in a child. Child's Nervous System. 24 pp. 1–2.
Rodriguez-Florez. N., Goktekin, O.K., Bruse, J.L., Borghi, A., Angullia, F., Knoops, P.G.M., et al., 2017. Quantifying the effect of corrective surgery for trigonocephaly: A non-invasive, non-ionizing method using three-dimensional handheld scanning and statistical shape modelling. Journal of Cranio-Maxillofacial Surgery. 45(3) pp. 387–94.
Refer your child to Mr Greg James
Use the form below to refer your child for treatment. A member of our team will be in touch within 2 working days.
Mandatory fields