A Miracle in Motion: Izz’s Triumph and Recovery from AADC
Two-year-old Izz from Saudi Arabia smiled and danced as his father sang to him, a joyful moment that reflected his remarkable recovery, that his parents described as a miracle. A warm atmosphere filled the Bumblebee Ward at Great Ormond Street Hospital (GOSH) as father and son connected in way that once wasn’t possible.
Although sitting independently, holding his head up, and dancing to music may seem like everyday milestones for most children, they were unimaginable for Izz just weeks earlier.
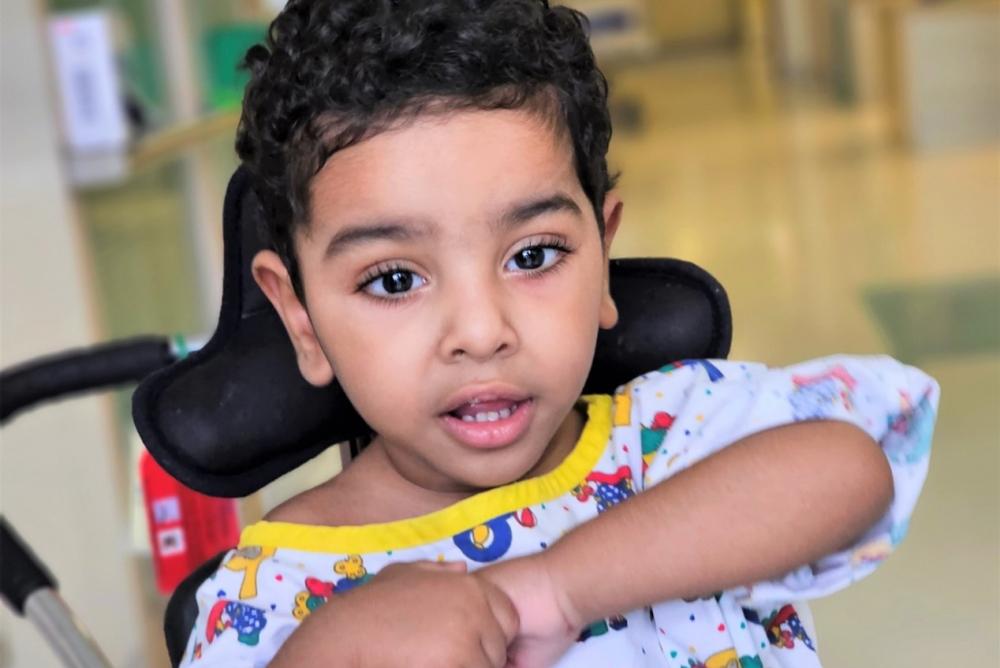
Izz was born after a normal delivery, with a slightly below average birth weight. and normal vital signs.
At 4-months old, however, things started to change. His dad, Fahad, said his son was not showing the same signs of development as other babies his age.
“He did not reach for things, nor was he able to hold onto them. He could not turn his head normally, he was always crying, and his mood was always down.’’
After having run a series of tests, doctors assured Izz’s parents that most of their son’s results were normal and their concerns could be attributed to slightly faltering growth.
AADC takes hold
At 7 months old, there was a major turn in Izz’s health, he started experiencing breathing difficulties and his parents found themselves rushing him to hospital almost every week, sometimes daily. They grew increasingly worried when Izz started struggling to swallow and his face would turn blue from choking. His breathing became more difficult, and seizures started happening regularly. Doctors still couldn’t figure out what was causing it. After a particularly scary episode, they decided to send his medical reports and samples to Germany, hoping to finally get some answers.
Two months later, Izz’s family received the news: he had a mutation in one of his genes that prevents his brain from making important chemicals like dopamine and serotonin. The condition is called Aromatic L-amino Acid Decarboxylase Deficiency, or AADC for short.
Professor Manju Kurian, Consultant Paediatric Neurologist at GOSH and a Professor of Neurogenetics at University College London (UCL) who specialises in looking after children with complex movement disorders, explains “Children that are affected by this condition have a reduced ability to produce two very important neurochemicals in the brain.
Firstly, serotonin and dopamine are important chemicals in the brain that control our movements, emotions and behaviour. Dopamine is also converted into other important chemical messengers, called epinephrine and norepinephrine that are very important in how we react to things around us. As a result of the inability to produce these very important brain chemicals, these children have developmental delay. Often, they have very little or no neurodevelopment and the majority of children can't lift their heads, let alone any further motor development. Most also have very complex abnormal movements known as dystonia (twisting postures) and chorea (excessive involuntary movements).’’

AADC care limits
Izz’s parents were on alert every day, taking turns day and night to care for him, battling the seizures, feeding challenges, and different breathing difficulties he was having.
“We had to organise our time, work, and everything we did to ensure that when something happened, we were there to relieve him of his pain or take him to the hospital as often was the case. We had even learned how to use oxygen tanks, saline drips, and how to help him inhale steam at home.’’ said dad Fahad.
After six months of dealing with Izz’s declining health, they went to see a doctor which prompted him to launch a nationwide search for similar cases in the hopes that they could better understand what is happening to Izz. The news came back that there were three other cases handled by a doctor in the capital, Riyadh.
When they arrived at her clinic, Izz had one of the most recognisable symptoms of AADC and some other movement and neurological disorders, an Oculogyric Crisis (OGC), where the eyes turn upward and stay that way for a while.
“When visual stimuli capture his attention, such as trees or lights and shiny objects, Izz would look up to see them and his eyes would stay up. It is one of the things which had worried us so much and we’d learned to stay on the lookout for.’’ As is often the case in Saudi Arabia, when a complex and rare case is identified, authorities explore the best treatment path available. In this case, it was determined the best option was to send Izz to GOSH in London.
Treatment journey at GOSH
Izz was 21 months when he arrived at GOSH where Professor Kurian and her team carefully reviewed every part of Izz’s case. “After we met Izz, we spent some time just confirming his diagnosis. We wanted to be absolutely sure. So, we undertook some tests, we reviewed his genetics, we reviewed his medication, and we were able to confirm a diagnosis of AADC deficiency.’’ Professor Kurian said.
Professor Kurian and her team then went on to have a very detailed discussion with his family about gene therapy, specifically Eladocagene Exuparvovec.
Gene therapy aims to address the root cause of the condition by delivering a working copy of the faulty gene directly into targeted areas of the brain. This allows brain cells to start producing the missing AADC enzyme, helping to restore the balance of dopamine and serotonin. For children, this can mean improvements in movement, development of new motor skills and, in some cases, the ability to achieve milestones such as sitting, standing or walking.
Understandably, the family were very anxious, but they were guided carefully through every step. They were taken through what would be required before the operation, what would happen during it, and what to expect afterwards. Professor Kurian explained that she believed Eladocagene Exuparvovec was the best option for Izz.
The family decided to proceed given what they understand about the nature of AADC deficiency and the fact most children don't even achieve head control.
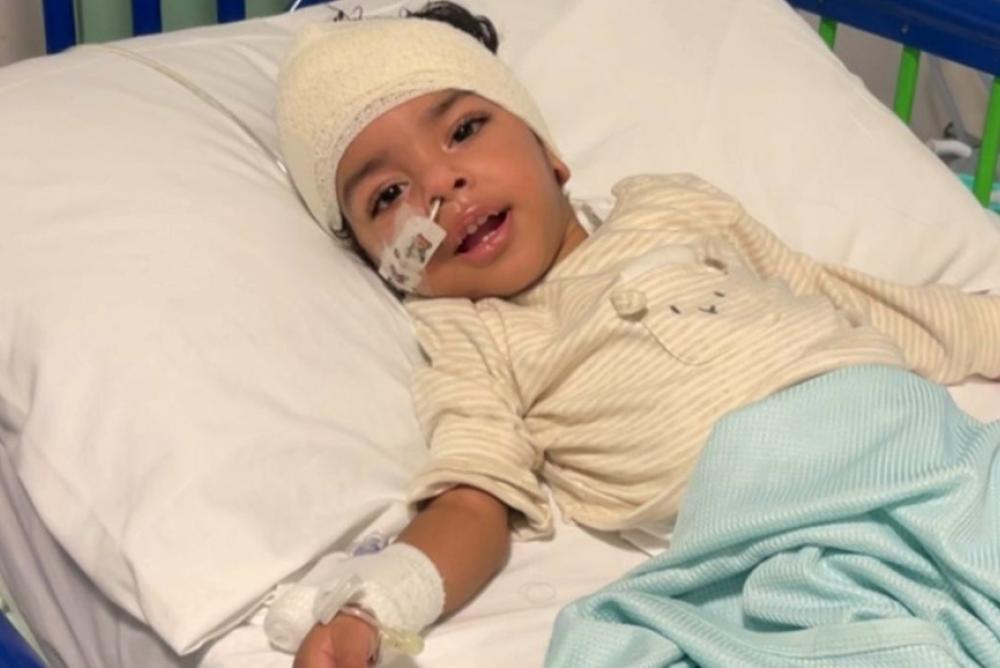
Professor Kurian added: “We spent some time working on making sure Izz was fit enough for the treatment, making sure that he was anaesthetically safe for the operation, that he would be able to tolerate a general anaesthetic, optimising his health, optimising his AADC medication and then he was ready to have the operation.’’
To deliver the gene therapy, surgery was required in which two small holes were drilled into Izz’s skull to access targeted areas of the brain. This was pre-planned as part of a meticulous treatment approach developed by Professor Kurian, Mr Kristian Aquilina (Consultant Paediatric Neurosurgeon), and the multidisciplinary team.
Mr Kristian Aquilina, Consultant Paediatric Neurosurgeon at GOSH, explains that they always have several discussions with families, before going through the surgery.
“Naturally, families can be somewhat apprehensive of a surgical procedure, but we sit down and explain to them what we plan to do. We show them the scans and explain the benefits on the one hand and the potential risks on the other. We explain that this is a safe and effective procedure and reassure families that we take all the precautions necessary to ensure maximal safety. This includes carrying out the procedure within the MRI scanner, to ensure that the drug is accurately injected in the correct places in the brain.”
Izz then went into surgery, which lasted 11 hours. “When I was told the details of the operation and how the surgery was carried out, I could not believe my ears. A very complex and intricate process where surgeons navigated with millimetric accuracy to inject the gene therapy.’’ Dad Fahad said.

Post-op care and recovery at GOSH
Prior to treatment, Izz has had bouts of muscle tension and oculogyric crisis that would last between six to eleven hours. Two months after the surgery he had only experienced one seizure which lasted eight minutes, he continued to have short oculogyric crisis, but these were much better than before surgery when they would last for hours.
The team, and Professor Kurian and Mr Aquilina, were always attentive in following up, at all hours and without fail. Professor Kurian, as the adage back home goes, is like a guiding fire atop a mountain. Anything I requested, she swiftly assessed and responded to,’’ Fahad said.
“The nurses, doctors, and Professor Kurian at the top formed a pyramid of care that flawlessly and relentlessly kept abreast of process at every turn. I had been with Izz to many hospitals almost weekly and sometimes even daily, but here at GOSH, whatever I requested or made a remark about regarding Izz’s daily status was met with a respectful manner, accommodating attitude, and assessed in a professional manner. My heartfelt thanks to all of them from the top of the pyramid to the bottom.’’
Izz now has full head control and can sit independently, two huge milestones that mark the progress of his treatment. Instead of waking up at all hours of the night now he sleeps soundly through the night. He is able to hold onto things and play with toys and he can even recognise and tell apart different members of the family when they call to check on his progress.
“The feeling of him holding my hand, which he could not do before the treatment, and watching him start to speak was a dream. The first time I heard the word ‘baba’ (Arabic for dad) was when he was 2 years old. The feeling was indescribable.’’
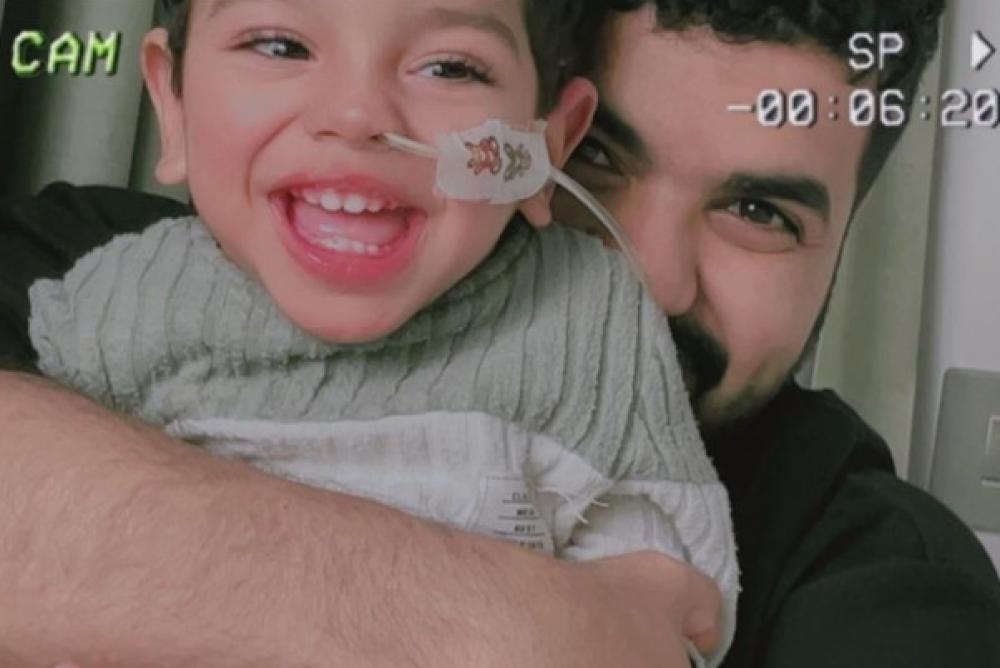
Izz’s treatment plan also includes physical therapy to address the effects of abnormal muscle tone before the surgery.
Dad Fahad said: “As the days go by and with the treatment and physical therapy things will get better. So far, his movement, sleep, mood, and emotions are better. A huge transformation took place from what he was he like before the treatment and what he is now. A 180-degree change. A miracle has happened here.’’
As Izz continues his treatment and follow-up care, his smile shines brighter than ever. His progress is a testament to the power of Eladocagene Exuparvovec, giving him the chance to achieve milestones once thought out of reach. His family remain hopeful and devoted, while his doctors continue to work to support him into his future.

